Your Body Has Been Warning You. Have You Been Listening?
Most serious diseases don’t arrive with a dramatic announcement. No sudden collapse, no obvious signal, no moment of clarity. They build quietly — and they warn you first. The trouble is that most of us don’t know what those warnings look like. And so we explain them away, press on, and book the appointment only when things have gotten considerably worse.
My aunt did exactly that. For nearly four months, she had a persistent cough — the kind that overstays its welcome long after any cold has gone. Dusty air, maybe. Seasonal change, probably. Work stress, almost certainly. Each explanation felt completely reasonable. Then she finally went to see a doctor, and the imaging revealed a shadow in her lung that had been quietly growing while life continued around it.
She’s alright. But it was far closer than it needed to be. And what strikes me most is that her body had been signalling the problem all along — it was just using a language she hadn’t been taught to read.
This article is about learning that language. The early warning signs of disease you should know are not obscure medical trivia. They’re physical, cognitive, and behavioural shifts that your body uses to communicate systemic stress — often months before anything shows up on a scan. Recognising them doesn’t require a clinical background. It requires attention, and it requires knowing what deserves more than a passing shrug.
What follows is not a hypochondria manual. It’s a practical guide to the twelve signals that medical literature consistently connects to serious but treatable conditions — along with a clear framework for what to actually do when you notice one.
| 📋 What You’ll Find in This Article ▸ The 12 early warning signs of disease clinicians flag most consistently ▸ Which symptoms should never be attributed to stress without proper testing ▸ A 5-step action plan for responding when something feels off ▸ An honest guide to when you need the emergency room versus your regular doctor ▸ How modern health technology is making early detection more accessible than ever |
The Real Reason We Miss the Warning Signs
There’s a version of this problem that’s easy to explain: people are busy, healthcare is expensive, and nobody wants bad news. That’s all true. But it doesn’t capture the full picture.
Life Is Loud. Symptoms Are Quiet.
The deeper problem is one of signal-to-noise. Fatigue, for example, is a genuine early indicator of thyroid failure, early-stage cancer, and uncontrolled diabetes. It’s also what happens when you sleep badly for a week. Your body can’t distinguish between those explanations when it sends the signal — and so neither can you, without the right framework.
We normalise our symptoms because normalising is the rational default. If something has an obvious explanation, you take the obvious explanation. That cognitive shortcut is usually right. But for a meaningful portion of people, it delays care by weeks, months, or longer.
One study in a major general medicine journal found that nearly seven in ten adults had sat with a worrying physical symptom for more than two weeks before contacting a doctor. The most common reason they gave was that they assumed the symptom would resolve on its own. For many, it did. But ‘it might go away’ is not a sufficient reason to ignore the body signals of serious illness — particularly when persistent symptoms are one of the most reliable early indicators available to you.
What ‘Hidden Disease’ Actually Means
Doctors use the phrase ‘hidden disease’ to describe conditions that progress silently through their early stages — not because they leave no traces, but because their traces are subtle enough to miss without awareness. Pancreatic cancer, pre-diabetic Type 2 diabetes, hypertension, early ovarian cancer, and chronic kidney disease all fall into this category. They are conditions that can take months or years to produce symptoms dramatic enough to demand attention.
But subtle does not mean absent. Even these conditions leave physical signals — shifts in energy, changes in appetite, minor but persistent alterations to normal body function. The early warning signs of hidden illness are there. They just require you to be paying attention, and to know what actually warrants a medical conversation rather than another week of waiting.
| Catching disease early is rarely a matter of luck. It’s a matter of knowing which signals your body sends — and taking them seriously when they appear. |
12 Early Warning Signs of Disease You Should Know
These twelve signs were selected for one reason: the medical literature consistently connects each of them to serious conditions that are significantly more treatable when identified at an early stage. None of them is a diagnosis on its own — a single symptom rarely is. But each one is a legitimate reason to pay closer attention, and in several cases, to book a medical appointment within the week.
This is the core of what the early warning signs of disease you should know actually look like in practice.
1. Fatigue That Doesn’t Shift With Rest
Not the tiredness that a decent night’s sleep fixes. This is fatigue that settles into your days regardless of how much you sleep — the kind that makes normal tasks feel like they’re being completed underwater. It’s dulling, persistent, and distinctly different from ordinary tiredness.
Clinically, unexplained fatigue lasting more than two weeks is a significant silent disease warning sign. It appears early in thyroid dysfunction (both overactive and underactive), iron-deficiency anaemia, uncontrolled Type 2 diabetes, chronic kidney disease, leukaemia, and several autoimmune conditions. When the body is fighting a systemic problem, it reroutes energy from normal daily function — and fatigue is often the first evidence of that rerouting.
| 🔎 When This Warrants Action ▸ Two or more weeks of fatigue with no clear cause — poor sleep, high stress, recent illness, or a demanding physical period — is worth flagging to a doctor. Bring a simple log: dates, severity on a 1–10 scale, time of day it’s worst. That information meaningfully speeds up the diagnostic process. |
2. Weight Changes You Haven’t Caused
The key word is ’caused.’ Losing weight because you changed your habits is expected. Losing 4–5 kilograms over six months with no change in diet or activity is clinically significant — and that distinction matters.
Unexplained weight loss is one of the early warning signs of hidden illness that physicians take most seriously across primary care. It’s a known feature of early-stage cancers (particularly gastrointestinal, lung, and lymphatic), hyperthyroidism, uncontrolled diabetes, and advanced Crohn’s disease. The body is burning through reserves faster than normal — and something is driving that process.
The reverse matters too. Sudden unexplained weight gain — especially when it comes alongside visible swelling in the lower legs or face — can indicate an underactive thyroid, early heart failure, or kidney-related fluid retention.
| 🔎 When This Warrants Action ▸ A shift of 4 or more kilograms over a few months with no dietary or lifestyle explanation deserves a blood panel. It’s a low-cost, high-yield first step. |
3. Pain That Keeps Coming Back With No Clear Cause
A single ache is rarely alarming. Pain that returns to the same location, at roughly the same intensity, without a mechanical cause — that’s a different matter.
Recurring headaches that behave differently from your usual pattern (different location, worse in the mornings, worsening when lying flat) can reflect elevated pressure inside the skull — a feature of several neurological conditions and some brain tumours. Persistent abdominal pain, particularly when it intensifies after eating or arrives in waves, is associated with early gastrointestinal cancers, inflammatory bowel disease, and chronic liver conditions.
Back pain that wakes you at night, that doesn’t respond to usual measures, or that travels down one leg with associated weakness is a different clinical category from the routine lower-back strain most people experience. It’s one of the body signals of serious illness that gets written off most often simply because back pain is so common — but frequency and seriousness are not the same thing.
4. Skin Changes — The Body’s Most Readable Diagnostic Panel
Your skin is more than a covering. It’s the most visible output of several internal organ systems, and it responds to internal stress in ways that are often detectable long before other symptoms emerge.
Jaundice — the yellowing of skin and the whites of the eyes — signals that the liver or bile ducts are struggling to process waste products. It requires medical attention the same week it appears. New pallor, particularly a sudden ashen tone in someone who has always had normal colour, can indicate anaemia or circulatory compromise.
And then there are changes to existing moles or the appearance of new lesions. Melanoma — among the most aggressive skin cancers if caught late, and among the most curable if caught early — is identified using the ABCDE framework: Asymmetry (one half doesn’t mirror the other), Border irregularity (edges are ragged or uneven), Colour variation (multiple shades of brown, black, or red in one mole), Diameter over 6 millimetres, and Evolution (any change in size, shape, or colour over six to eight weeks). A mole that meets any two of these criteria warrants a dermatology referral.
| 🩺 Simple Habit Worth Building ▸ Set a monthly phone reminder for a head-to-toe skin check. Photograph anything unusual. If the same spot looks different four weeks later, make an appointment. |
5. A Cough That Outlasts Its Welcome
A cough that arrives with a cold and lingers for a week or two afterwards is completely normal. The immune system takes time to clear residual inflammation. But a cough that continues for three or more weeks after any respiratory illness has resolved is a different clinical event — and it should be treated as one.
A persistent cough is one of the most documented symptoms your body is fighting disease. It’s the primary presenting complaint in a significant proportion of lung cancer diagnoses, and a key feature of COPD, pulmonary fibrosis, and cardiac failure in its early stages (where it often presents as a nocturnal dry cough or a cough that worsens when lying flat).
Any blood in a cough — even once, even a trace — is not a symptom to monitor. It’s a reason to call your doctor that day.
Breathlessness during activities that previously caused you none is in the same category. If climbing one flight of stairs leaves you noticeably short of breath when it didn’t last year, your heart or lungs are telling you something worth hearing.
6. Changes in Bowel or Bladder Function
Most people avoid this conversation. That avoidance is understandable, but it has real health consequences.
Colorectal cancer is among the most common cancers globally, and it is also among the most survivable when identified at an early stage. Its earliest indicators are almost entirely bowel-related: a change in stool consistency or frequency that persists beyond four weeks, rectal bleeding in any amount, a feeling of incomplete emptying after a bowel movement, or stool that is significantly narrower than usual. These are early warning signs of disease you should know — not subjects to file under ‘probably nothing.’
On the urinary side, blood in the urine has no benign explanation. Even a single episode warrants a call to your doctor the same day. Urinating frequently through the night combined with unusual thirst is the classic early presentation of uncontrolled diabetes — and catching it before it progresses has significant long-term health implications.
That was the most uncomfortable section. This next one is the check most people forget to schedule.
7. Lumps, Swellings, or Unfamiliar Thickenings
Not every lump is dangerous. The body is full of benign cysts, lipomas, and lymph nodes that are minding their own business. But a lump that was not there before, that is growing, and that is painless and firm rather than soft and tender, is worth having examined.
Enlarged lymph nodes in the neck, armpits, or groin are the body’s immune response to infection in the majority of cases. When they persist for more than two to four weeks after an infection has resolved, are hardening or increasing in size, and are not tender to the touch, they become one of the most significant silent disease warning signs for lymphoma and other blood cancers.
Breast tissue changes — in any person, regardless of gender — should always be reported. Testicular changes, abdominal swelling without obvious dietary cause, and any new palpable mass anywhere on the body deserves a clinical assessment. The examination takes five minutes. The information it provides can be life-altering.
8. Persistent Low-Grade Fever
A fever above 38°C with a clear infection behind it — flu, a UTI, an ear infection — is a normal immune response. What is clinically different is a temperature that hovers persistently between 37.5°C and 38.3°C for two or more weeks without a detectable cause.
This pattern is one of the more significant early warning signs of disease you should know — specifically for haematological malignancies including lymphoma and leukaemia, several autoimmune conditions, and certain chronic infections. When this low-grade fever is accompanied by drenching night sweats and unintentional weight loss of more than 10% of body weight, doctors refer to this cluster as ‘B symptoms’ — three co-occurring indicators that trigger urgent haematology referral in most clinical guidelines.
| 🔎 When This Warrants Action ▸ Take your temperature at the same time each evening for fourteen days. If it consistently exceeds 37.4°C without a clear infectious cause, bring that log to a medical appointment. Two weeks of temperature data carries more diagnostic weight than a single reading. |
9. Cognitive Changes — Brain Fog, Memory Gaps, Concentration Loss
There’s a meaningful clinical difference between forgetting a name you’ll remember in an hour and experiencing a persistent cognitive fog that makes ordinary thinking feel effortful. The first is normal. The second deserves investigation.
New-onset brain fog — described as difficulty concentrating, losing words mid-sentence, struggling to follow conversations, or feeling consistently slower than usual with no obvious cause — is one of the frequently overlooked body signals of serious illness. It features in early presentations of hypothyroidism, Lyme disease, autoimmune encephalitis, severe anaemia, and uncontrolled diabetes.
Sudden onset of confusion, disorientation, or inability to speak normally in someone who was entirely lucid moments before is a neurological emergency. Call for help immediately. Do not drive the person to hospital yourself.
10. Extreme Thirst Combined With Frequent Urination
When blood glucose levels climb beyond what the kidneys can manage, the body attempts to flush the excess through urine — which requires significant water. The result is a self-reinforcing cycle: high glucose drives excessive urination, which produces intense thirst, which drives increased fluid intake, which produces more urination.
This pairing is the most textbook presentation of early-stage Type 1 and Type 2 diabetes, and it’s one of the early warning signs of hidden illness that people most consistently explain away. ‘I’ve just been drinking a lot of coffee’ or ‘it’s been a hot week’ — except that the symptom doesn’t improve when conditions change.
When this symptom cluster arrives alongside unexplained fatigue and visual blurring, a fasting blood glucose test and HbA1c (a three-month average blood sugar reading) should happen within the same week. Early intervention in diabetes changes its long-term trajectory significantly.
11. Heartburn That Won’t Respond to Medication — Or Difficulty Swallowing
Occasional heartburn after a large meal or a glass of wine is one of the more universal human experiences. Two or more episodes per week, persisting despite over-the-counter antacids, lasting for more than a month — that is a different clinical picture.
Untreated chronic acid reflux causes progressive damage to the oesophageal lining, leading to a precancerous condition called Barrett’s oesophagus. This isn’t inevitable — it’s preventable with early management. But only if the symptom is taken seriously rather than managed indefinitely with antacids from a pharmacy shelf.
Difficulty swallowing — the sensation of food sticking or sitting in the chest rather than passing — is among the earliest early warning signs of disease you should know for oesophageal cancer. Oesophageal cancer caught at Stage 1 carries a five-year survival rate of over 80%. Caught at Stage 4, that figure drops below 5%. The difference is almost entirely a matter of whether the swallowing difficulty was investigated early.
12. Unexplained Bruising or Wounds That Are Slow to Heal
Easy bruising — the kind that appears from a light knock that would previously have left no mark — becomes more common with age and with certain medications. But bruising that appears with no impact at all, or that spreads to an area much larger than the force that caused it could explain, is worth flagging.
This is a consistent silent disease warning sign for platelet disorders, leukaemia, and liver disease — conditions that impair the blood’s ability to clot normally. Spontaneous nosebleeds, prolonged bleeding from minor cuts, and bleeding from the gums without dental cause fall into the same category.
Wounds on the lower legs or feet that fail to heal normally over two to three weeks are a key early sign of uncontrolled diabetes and peripheral vascular disease — both conditions in which poor circulation starves the tissue of the resources it needs to repair.
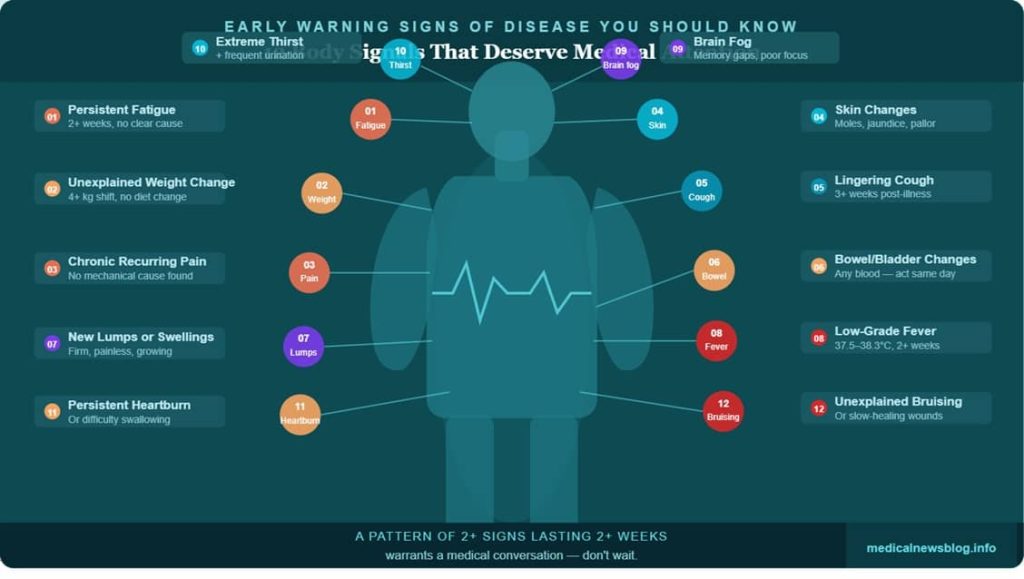
| ⚡ Quick Reference: Early Warning Signs of Disease You Should Know ▸ 1. Fatigue that doesn’t shift with rest — lasting 2+ weeks ▸ 2. Unexplained weight change of 4+ kg in either direction ▸ 3. Recurring pain with no mechanical cause ▸ 4. Skin changes — jaundice, mole changes, new pallor ▸ 5. Cough lasting 3+ weeks, or any blood in cough ▸ 6. Changes in bowel or bladder habits, any blood in either ▸ 7. New lumps, swellings, or thickenings anywhere on the body ▸ 8. Low-grade fever (37.5–38.3°C) persisting 2+ weeks ▸ 9. New brain fog, memory gaps, or concentration difficulty ▸ 10. Extreme thirst + frequent urination together ▸ 11. Persistent heartburn unresponsive to antacids, or difficulty swallowing ▸ 12. Unexplained bruising or slow-healing wounds |
If Your Risk Profile Is Higher, These Signs Matter More
The twelve signs above matter for everyone. But for certain groups, the same symptom carries a heavier clinical weight — because it’s arriving in a context where the probability of a serious underlying cause is meaningfully higher. If you sit in any of these categories, the early warning signs of hidden illness deserve your full attention rather than the benefit of the doubt.
Anyone Over 40
The biology is straightforward: after the age of 40, the body’s cell-repair mechanisms, hormone regulation, and immune surveillance all become less efficient. Conditions including cardiovascular disease, Type 2 diabetes, thyroid dysfunction, and the most common cancers become statistically more prevalent. The symptoms your body is fighting disease at this stage can be subtle — and are far more likely to be written off as normal ageing. Don’t let ‘that’s just your age’ be the end of the conversation with your doctor or yourself.
Anyone With a Significant Family History
If a first-degree relative (parent or sibling) has had colorectal cancer, breast cancer, ovarian cancer, early-onset cardiovascular disease, or Type 2 diabetes, your own risk profile is elevated above the general population. Your screening should start earlier than the standard age guidelines suggest, and the early warning signs of disease relevant to your family’s specific pattern deserve heightened attention.
Anyone Under Sustained Chronic Stress
This is the group most likely to dismiss their symptoms as ‘just stress’ — and sometimes that’s accurate. But chronic psychological stress suppresses immune function, drives systemic inflammation, disrupts sleep quality, and elevates cortisol in ways that accelerate metabolic and cardiovascular disease progression.
More practically: stress produces the same symptoms — fatigue, weight change, cognitive fog, disrupted digestion — that characterise many of the early warning signs of disease you should know. This overlap means stressed individuals are more likely to attribute serious physical symptoms to emotional causes. If you’re under significant sustained pressure, be more vigilant about physical symptoms — not less.
If you recognised yourself in any of those groups, the next section is particularly for you.

What to Do When Something Doesn’t Feel Right: A Practical Framework
Recognising the early warning signs of disease you should know is the first move. Acting on that recognition is the second. Here is a five-step process that takes you from ‘I’ve noticed something’ to ‘I’m doing something about it’ without either catastrophising or dismissing.
- Write it down specifically. Note the symptom, when it started, how frequently it occurs, what makes it better or worse, and whether it’s changing over time. Memory is unreliable over weeks — a written log is not.
- Cross-reference with the 12 signs above. Is this symptom new? Persistent? Does it match one of the clinical patterns described?
- Assign an urgency level. Use the table below. Is this a same-day emergency, a this-week appointment, or something to monitor for a further two weeks before acting?
- Prepare for your appointment. Bring your written symptom log, a full list of current medications and supplements, and a note about any relevant family history. These three things improve consultation quality significantly.
- Follow up if your concern isn’t resolved. If you leave an appointment without a clear explanation and still feel that something is wrong, it’s entirely reasonable to ask: ‘What have we ruled out, and what hasn’t been tested yet?’ A second opinion is always available to you.
Emergency Room vs. GP Appointment — Know the Difference
| Go to Emergency Room Today | Book a GP Appointment This Week |
| Chest pain with breathlessness, sweating, or arm pain | Fatigue lasting more than two weeks with no clear cause |
| Sudden severe headache unlike any previous | Unexplained weight loss of 4+ kg |
| Stroke signs: facial droop, arm weakness, slurred speech | Cough persisting more than three weeks |
| Coughing or vomiting blood | Unusual or changing skin lesion |
| Acute confusion or loss of consciousness | Persistent low-grade fever with no infection |
| Large volume blood in stool or urine | New lump or thickening anywhere |
Screenshot this table. Keep it on your phone. You won’t regret having it available when you actually need it.
Preventive Screening: Know What to Book and When
| Age Range | Screening to Schedule |
| 20–39 | Annual blood pressure; cholesterol every 4–6 years; fasting glucose if risk factors present; skin check |
| 40–49 | Annual blood pressure and lipid profile; fasting glucose and HbA1c; mammogram discussion (women); colorectal cancer baseline; PSA discussion (men from 45) |
| 50–64 | Colonoscopy every 10 years; bone density scan; annual comprehensive metabolic panel; low-dose CT chest if heavy smoker |
| 65+ | All of the above plus annual medication review, cognitive screening, and fall-risk assessment |
What Modern Technology Is Adding to Early Detection
The practical capacity to catch disease early has improved substantially in the last decade. Some of that improvement comes from better clinical protocols. A growing portion of it comes from technology.
AI Diagnostic Tools
Machine learning algorithms trained on large clinical datasets are now identifying early-disease patterns in imaging, blood work, and electrocardiograms that human clinicians might not detect in early-stage presentations. To understand how these systems work in practice, read our detailed guide to AI-powered diagnostic tools that are already detecting disease earlier — including real-world examples from cardiology and oncology departments already using them.
For patients, this means that the early warning signs of disease you should know are increasingly being caught — provided you’re showing up for routine screening. The technology exists. The bottleneck is still the gap between symptom onset and the decision to seek care.
Wearable Monitoring
Consumer wearable devices now offer continuous heart rate monitoring, blood oxygen tracking, irregular rhythm detection, and sleep stage analysis. These tools don’t replace clinical assessment — but they can surface body signals of serious illness that would otherwise go unnoticed: a persistent resting heart rate that has been 15 beats per minute higher than your normal baseline for three weeks; blood oxygen readings that dip below 94% regularly during sleep; a heart rhythm irregularity flagged during an afternoon walk.
Remote patient monitoring programmes — increasingly covered by Medicare and similar schemes — extend this capability further, allowing clinicians to receive real-time physiological data from patients managing chronic conditions outside a clinical setting. The benefits of remote patient monitoring for chronic disease management go well beyond convenience — they include earlier detection of deterioration, fewer emergency admissions, and measurably better patient outcomes.
The Part Technology Can’t Replace
All of this is genuinely useful. And none of it matters unless you’re paying attention in the first place. Technology can process data, flag patterns, and surface anomalies. But it depends on you noticing that something has changed — and doing something about it.
The most powerful early-detection tool available to you today is not an algorithm. It is your own consistent, honest attention to how your body feels — and the willingness to act on what you notice.
Common Questions — Answered Directly
These are the questions people ask most often on this topic — in search engines, to voice assistants, and in doctors’ waiting rooms. The answers are kept short and direct.
What are the early warning signs of disease you should know?
The most important early warning signs of disease you should know are: persistent unexplained fatigue, unexplained weight change, recurring pain without a mechanical cause, new or changing skin signs, a cough lasting more than three weeks, any blood in stool or urine, a new unexplained lump, persistent low-grade fever, new cognitive fog, extreme thirst with frequent urination, persistent heartburn or swallowing difficulty, and unexplained bruising. A pattern of two or more of these lasting more than two weeks warrants medical assessment.
How do I know if my body is fighting a hidden disease?
Watch for persistent changes from your normal baseline — not one-off events. Symptoms your body is fighting disease tend to be consistent, gradually worsening, and resistant to the simple explanations you’d normally apply. The two-week rule is a useful practical threshold: if the same symptom is still present two weeks after you first noticed it, with no obvious cause and no improvement, book an appointment.
When should I see a doctor about a symptom?
For emergency symptoms — chest pain, stroke signs, blood in cough, loss of consciousness — go to the emergency room today. For persistent symptoms that don’t resolve within two weeks with no clear cause, book a GP appointment within the week. Do not use ‘it will probably go away’ as an indefinite strategy for symptoms that have already been present for two weeks or more.
Can stress cause symptoms that look like serious disease?
Yes — and this creates a genuine diagnostic challenge. Chronic stress produces fatigue, weight changes, brain fog, digestive disruption, and headaches that closely mirror several hidden disease symptoms. The clinical principle is that stress should be a diagnosis of exclusion — meaning physical causes should be actively ruled out through testing before symptoms are attributed to stress. If your doctor suggests stress without ordering any tests, it’s reasonable to ask what conditions have been excluded.
Which diseases show almost no early symptoms?
Several of the most significant: hypertension (the ‘silent killer,’ often producing no symptoms until it causes a cardiac event or stroke), pre-diabetic and early-stage Type 2 diabetes, pancreatic cancer (which rarely causes pain until advanced), early-stage ovarian cancer, and chronic kidney disease. This is the strongest argument for routine preventive screening — many of these conditions are detectable through standard blood tests and imaging long before they become symptomatic.
Are AI symptom checkers reliable?
As a starting point, yes — with clear limits. AI symptom checkers can help you decide whether a symptom pattern warrants a medical conversation and can provide useful context for what questions to ask. They cannot diagnose, they cannot account for your full medical history, and they should not replace clinical assessment. Use them to inform your decision about whether to book an appointment — not as a substitute for booking one.
Can children show early warning signs of hidden disease?
Yes. Children can show early warning signs of disease — and in some respects they are harder to identify because children may not be able to articulate what they’re experiencing. Key signals in children include unexplained weight loss, persistent fatigue that affects normal activity levels, bone pain that wakes them at night, easy bruising, pallor, and persistent fever. Any of these lasting more than two weeks in a child warrants a paediatric consultation.
Final Thought: Pay Attention — It’s Worth Your Time
My aunt is doing well. The condition found in her lung was caught early enough to manage effectively. She doesn’t call it lucky. She calls it ‘finally going to the doctor.’ That’s the whole story, really.
The early warning signs of disease you should know are not meant to send you into a spiral of anxiety every time you feel tired. They’re meant to give you a more accurate internal framework for distinguishing between ‘my body needs rest’ and ‘my body needs a doctor.’
You don’t need medical training to notice that your energy has been flat for three weeks with no explanation. You don’t need clinical knowledge to see that a mole on your arm looks different from six months ago. What you need is the habit of paying attention — and the understanding that acting on what you notice is not an overreaction. It’s exactly what you’re supposed to do.
The gap between ‘I noticed something was off’ and ‘I did something about it’ is where health trajectories are made or broken. Your body has been communicating with you all along. Now you know what it’s been saying.
The early warning signs of hidden illness are not dramatic. They’re quiet, persistent, and easy to explain away — until the moment they aren’t. Learn the twelve signs. Pay attention to your baseline. Act on changes. And go to the doctor before you feel like you absolutely have to.
| The best time to find a disease is before you feel sick. The second best time is the moment something in your body tells you that it’s there. |
| 📬 Continue Reading on medicalnewsblog.info ▸ AI Health Diagnostics: What Every Patient Needs to Know Now ▸ Benefits of Remote Patient Monitoring: 5 Key Facts ▸ How medical digital twins are changing personalised disease prevention — a full explainer on virtual patient models that simulate disease progression before symptoms appear.▸ Healthcare Innovation: Future Trends and Patient Care Strategies ▸ Subscribe to our weekly health newsletter — evidence-based updates, no noise. |
References & Evidence Base
This article was written to editorial health journalism standards. Evidence base includes:
- World Health Organization — Global Cancer Statistics (GLOBOCAN 2022)
- Centers for Disease Control and Prevention — Chronic Disease Prevention and Screening Guidelines
- National Institutes of Health — Early Detection Research Network
- American Cancer Society — Cancer Signs and Symptoms Clinical Guidance
- Mayo Clinic — Fatigue: Clinical Causes and Evaluation
- Journal of General Internal Medicine — Symptom Reporting Delays in Primary Care Patients
- The Lancet — Pancreatic Cancer: Early Detection and Survival Outcomes
- British Medical Journal — Unexplained Weight Loss in Primary Care Settings
- National Cancer Institute — Melanoma Detection: ABCDE Criteria
- Diabetes UK — Pre-Diabetes Recognition, Diagnosis and Early Intervention
| About This Article Written by the medicalnewsblog.info Editorial Team. This content is for general health education only and does not constitute medical advice. Always consult a qualified healthcare professional for any symptoms or medical concerns. |

